What is Acne?
 Acne vulgaris is a frequent skin disorder that is typically seen in teens of both sexes but also can affect adults of all ages. Acne is found in nearly 90% of individuals at some time during their lives.
Acne vulgaris is a frequent skin disorder that is typically seen in teens of both sexes but also can affect adults of all ages. Acne is found in nearly 90% of individuals at some time during their lives.
It is characterised by lesions that are commonly called comedones or pimples; their distribution is bilateral and symmetrical affect face, neck, chest, back, and shoulders.
The pilosebaceous unit is the target organ in acne. This structure includes the gland that produces oil or sebum (sebaceous gland) that keeps the skin moist, and the follicle where hair grows (hair follicle). These structures share a canal, which opens onto the skin surface (pore).
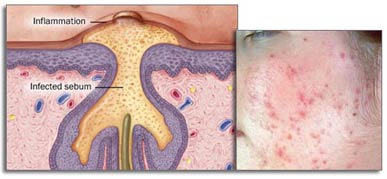
When sebum secretion is excessive and the pore is blocked by dead skin cells, the pilosebaceous unit becomes clogged and Acne develops. This initial lesion is called a comedone.
Bacteria that normally live on the skin and thrive on the sebum produced by sebaceous glands (Propionibacterium acnes) can build up and trigger inflammation, causing progression to papules, pustules, and in severe cases, nodules and cysts (large, painful bumps under the skin’s surface) which often can lead to scarring.
Hormones (androgens) play an important role in the development of acne since they directly stimulate sebaceous glands.
Comedones: Are a clogged hair follicle within the skin.
Whiteheads: Are closed comedones, sebum becomes trapped below the skin surface.
Blackheads: Are open comedones that are exposed to air. The exposure creates an ooxidisation of the contents creating its black colour.
Inflammatory Acne:
Occurs when there is a break in the follicular wall
- Papules: Are red, tender but do not have a head.
- Pustules: (pimples) Develop from papules- and have a head.
- Nodules: (inflamed bumps) Firm, large, red, painful, often cause scarring.
- Cysts: These are large pus filled lesions formed as a result of a severe inflammatory reaction and very often lead to scarring.
Residual Lesions:
- Hyperpigmentation
- Scarring: Atrophic: icepick, rolling or boxcar scarring
- Hypertrophic: keloids
Acne Is Not:
- It is not caused by poor personal hygiene
- It is not a contagious disease.
- Blackheads (open comedones) are black because of oxidized skin pigment melanin, not dirt and cannot be washed away.
- Greasy food and chocolate does not cause or worsen acne. However, products with these ingredients often contain a high glycemic load that can exacerbate acne.
Acne Is:
- Acne is treatable.
- Is a genetic predisposition.
- Androgens are a causative factor in acne, yet most acne patients do not typically have significant endocrine abnormalities.
- Hormonal changes are related to acne development which flares at the onset of puberty, before menstruation, during pregnancy, perimenopause, with some types of hormonal birth control, in association with hormonal disorders (polycystic ovarian syndrome, Cushing’s Syndrome, among others).
Acne Exacerbating Factors:
- Systemic medications: lithium, phenytoin, steroids, halogens, androgens, iodides, bromides, danazol.
- Topical agents: steroids, tars, ointments, oily cosmetics.
- Mechanical pressure or occlusion, such as leaning face on hands.
- High levels of humidity and sweating.
- High-starch foods (high glycemic load diets) as well as dairy products.
Treatments
General Recommendations:
- Do not scrub the skin with harsh soaps, washcloth or sponge; this irritates the skin and makes the acne worse
- Lesions should not be squeezed, scratch or picked. This can cause scarring.
- Cosmetics should be ‘oil-free’ or ‘Non-Comedogenic’
Pharmacological Therapies
- Topical Medications: Retinoids (adapalene, tazarotene, tretinoin), antibiotics (clindamycin, erythromycin), benzoyl peroxide, azelaic acid, dapsone.
- Oral medications: Oral antibiotics: (tetracycline, doxycycline, minocycline clindamycin, erythromycin), antiandrogens: (cyproterone acetate, spironolactone), retinoids: (isotretinoin – sexually active adolescent females without an effective birth control method and pregnant women should NOT take Accutane as it causes severe birth defects).
- Chemical Peels: Salicylic acid, lactic acid, retinoic acid
- Light-Based Therapies: LED (blue light), Photodynamic Therapy.
What is Rosacea?
Rosacea is a very common skin condition featuring flushing, permanent reddening, small pimples (with no blackheads) and visible blood vessels on the nose, cheeks, forehead and chin. Other features may be rough, red skin plaques, swelling or thickening of the skin, especially the nose (a condition known as rhinopyma) It can also affect other areas such as the scalp, ears, neck, chest, back and eyes. Symptoms may include burning or stinging, dry skin and watery or bloodshot eyes.
Rosacea is typically seen in fair-skinned women, but can also affect men who tend to develop more severe symptoms.
Rosacea is NOT an infection, (it is NOT a contagious skin condition).
Although rosacea papules resemble acne pimples, they are unrelated diseases.
- Erythematotelangiectatic: Characterized by facial redness, swelling, red blood vessels, rough patches, stinging sensation.
- Papulopustular: Persistent facial redness, presence of bumps or pimples (papules or pustules). It is often seen in combination with symptoms of erythematotelangiectatic type.
- Phymatous: Thickening skin, irregular surface, nodularities and enlargement (often affecting nose but also chin, forehead, cheeks or ears). It may appear after or in combination with symptoms of erythematotelangiectatic and papulopustular types.
- Occular: Foreign body sensations in the eye, burning or stinging, dryness, itching, ocular light sensitivity, blurred vision, telangiectasias of the sclera or other parts of the eye, or periorbital swelling. It may occur with or without other symptoms of rosacea.
- Closeness to hot sources such as stoves, ovens, etc
- Sun exposure, extreme temperatures (heat, humidity, cold) as well as abrupt changes in temperature and wind
- Hot drinks (coffee, tea) and hot food (soup)
- Spicy food, aged cheeses, chocolate, alcoholic drinks
- Intense exercise, anxiety, emotional stress
- Menopause
- Topical steroids (long-term use) and certain medications
Although there is no cure for rosacea, early diagnosis and prompt treatment prevents deterioration and improves facial appearance.
General Recommendations
- Treat your skin gently, protect it from direct cold, wind and sun exposure
- Use gentle skin care products (avoid products containing alcohol, menthol, exfoliating agents, fragrances)
- Avoid topical corticosteroids.
- Cosmetic Camouflage products (green-tinted make-up) may help minimize red tones in the skin
Specific Rosacea Treatments
- Topical Medications: metronidazole, clindamycin, eythromycin, benzoyl peroxide, sulfur
- Oral Medications: tetracyclines, erythromycin, metronidazole, retinoids
- Light Source Devices: IPL (Intense Pulse Light) and vascular-specific laser treatments can reduce the appearance of facial redness and visible blood vessels. Resurfacing lasers,eg. fractional CO2, can be useful in treating skin thickening lesions (rhinophyma).
